What about those psychedelics?
What about those psychedelics?
Psychedelic medications and therapies have become a pervasive meme recently. What is all the buzz about? For starters, the fields of psychiatry and psychology have been pretty underwhelming in the last several decades, leading to more interest in non-pharmacologic and non-talk therapy options. Many treatments that held promise have either not held up to the test of a clinical trial, or worse, have been marketed in spite of their failures (I am thinking about Robert Whitaker’s book, The Anatomy of an Epidemic, reviewed here).
Patients have been tapping into increasingly “woo-woo” (my favorite options, usually!) therapies because they often have minimal side effects, are less expensive and more accessible, and people feel better. Examples include neurofeedback, sound/vibration healing, shamanic journeywork, forest bathing, and a host of botanical medicines. Psychedelics are arriving on the scene after the tireless efforts of Rick Doblin and MAPS who have funded research and conducted clinical trials in the face of opposition from federal agencies induced by decades of stigma related to the war on drugs.
Because of the high quality research done by MAPS and other centers around the world like Imperial College with Robin Carhart-Harris, the medical community has been forced to look more openly at the benefits of psychedelics, particularly when compared to traditional medical approaches to conditions such as PTSD and treatment-resistant depression. One thing I love about psychedelic research is the ability of this therapy to transcend conflict, such as political disagreements. I think this is driven by the fact that PTSD and serious depression, suicidal ideations and crippling anxiety are known to all, regardless of race, creed, religion, political persuasion or other identities.
What’s the evidence for psychedelics?
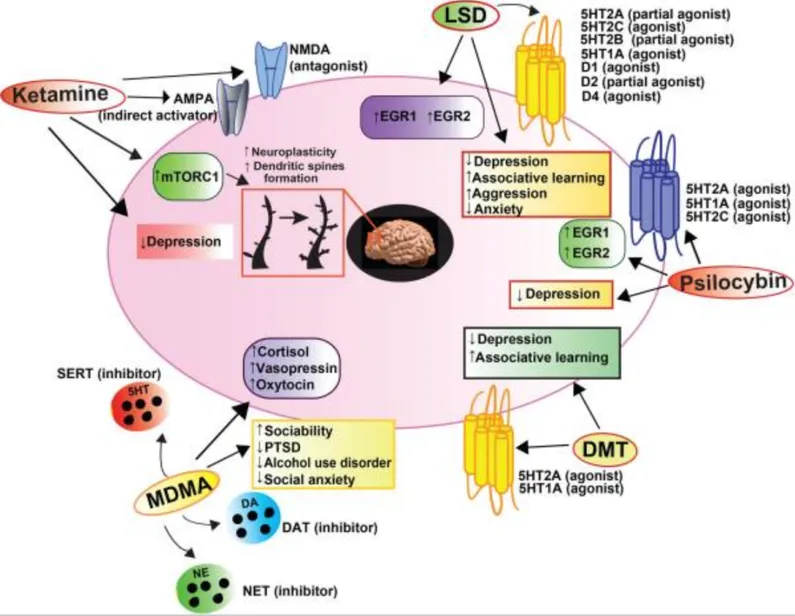
Various psychedelic medications have been studied, some of which enhance feelings AKA empathogens, and some of which enhance fantasy, such as ketamine, LSD and ayahuasca. A great introduction to these medicines is The Healing Journey, by the late psychedelic researcher Claudio Naranjo, a Chilean psychiatrist also known for his work using the Enneagram.
MDMA has been shown to actually help patients with severe PTSD in such a way that they no longer meet criteria for the disorder. In one of the clinical trials, 88% of patients treated with MDMA in 3 sessions had significant improvements and 67% no longer met the criteria for PTSD. In comparison, 32% of the patients who got placebo in this study no longer met criteria for the disorder.
Ketamine, the only currently legally available hallucinogen, has prompted the start of many ketamine clinics nationally. It appears to have rapid impacts on depression and suicidal ideation but varies in how long the improvements last. There are still lots of questions about how long its safe to use, and like all of these medications there remain many unanswered questions about how it actually works. However, compared to many available agents, the effectiveness is so superior that they have ended studies early because it would have been unethical to continue given the effectiveness of the treatment of ketamine over the comparison drug. So far, in severe, chronic PTSD, a standard protocol of 6 infusions done over 2 weeks had an effect lasting an average of about 4 weeks. People considering ketamine for their treatment options just have to be aware of the potential to need ongoing treatment in order to maintain their improvements.
Ketamine is a powerful catalyst that may help provide energy for change or reduce inner barriers to change. By working within the carefully curated container at Mindstream, clients receive preparation, integration and medicine session support that helps anchor the awarenesses that arrive using this approach.
In short, there’s some good reason for the hype around psychedelics. They aren’t wonder drugs, but they are way more effective in trials than what’s currently marketed. Particularly in a time globally in which mental health symptoms are at an all time high, these options for some “one and done” therapies, or “a couple and done” are appealing. The next challenge is that these could be accessible, both financially and logistically. Here’s to cures without many side effects, that possibly even fill your heart with joy!


